Meningococcal disease
Key facts
-
Meningococcal disease can cause inflammation around the brain (meningitis) and blood poisoning (septicaemia).
-
Vaccines are the best way to protect your child against meningococcal disease.
On this page
- What is meningococcal disease?
- What will happen to my child if they catch meningococcal disease?
- What vaccine will protect my child against meningococcal disease?
- When should my child be vaccinated?
- How does the meningococcal vaccine work?
- How effective is the vaccine?
- Will my child catch meningococcal disease from the vaccine?
- What are the common reactions to the vaccine?
- Are there any rare and/or serious side effects to the vaccine?
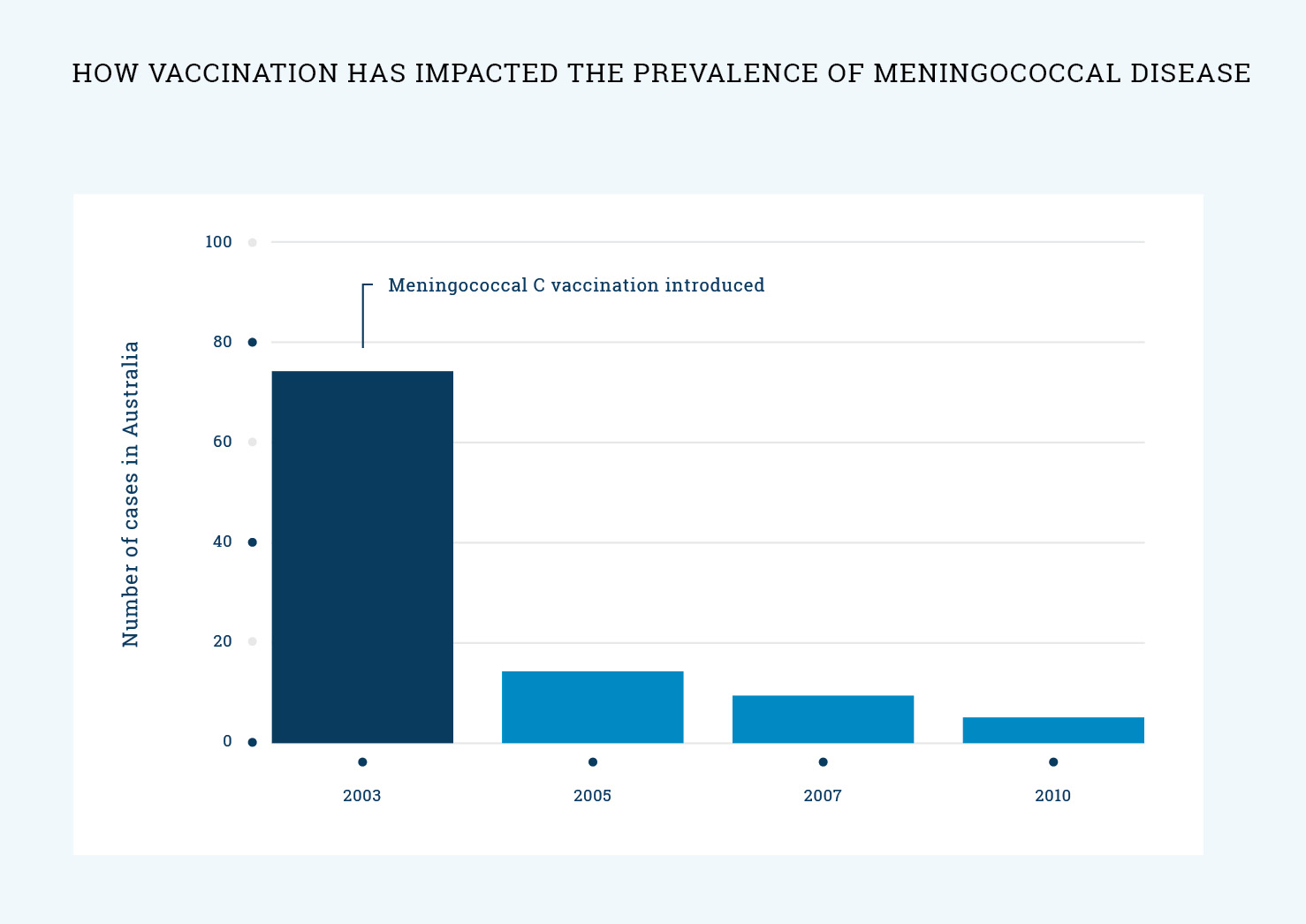
- What impact has vaccination had on the prevalence of meningococcal disease?